Are you, or your female clients struggling with all three?
Article by Gill Cummings-Bell BA (Hon’s). M.Sc. PGCE. MBA
Hypothyroidism and menopaus have a connection. Many women do not realise that there is an overlap between post menopausal symptoms and the symptoms of hypothyroidism. Hypothyroidism can increase or worsen symptoms of menopause. A research study published in the Journal of Thyroid Research reported that there is ‘evidence that oestrogen may have a direct action in human thyroid cells’, further research showed that women with a thyroid disorder and severe menopause experienced improved symptoms after getting treated for the thyroid disorder. These symptoms are commonly seen in both menopause and hypothyroidism. They are similar but also distinct
| Symptoms of Menopause | Symptoms of Hypothyroidism |
|---|---|
| irregularities in the lower urinary tract, such as frequent urination or excessive urination at night | higher levels of blood lipids, such as triglycerides and cholesterol |
| disturbed sleep | increased sensitivity to cold |
| problems focusing and learning | slower heart rate |
| changes in energy or feelings of fatigue | poor memory |
| changes in body weight, such as a sudden increase in weight | persistent fatigue or feelings of being tired |
| vulvovaginal atrophy and dryness | increase in body fat |
| cessation of menstrual cycles | weakness in muscles and joints |
| mood swings | thinning of head hair |
| hot flushes and night sweats | depression or sadness |
| hoarseness | |
| dry, chapped skin |
Hypothyroidism can also significantly increase the risk of complications during menopause. The AACE states that millions of women with menopause symptoms could be suffering from thyroid disease and not realise it. There is over 500 million women in the world who are post-menopausal and this is expected to increase to over 1.1 billion by 2025. Only 1 in 4 women actually speak to their GP about menopause. Although the two conditions are connected they are diagnosed and treated differently therefore developing a greater understanding of both conditions is necessary for us to truly help our female clients.
Many of you as female trainers or male trainers with female clients, will read this article and relate to body changes your clients or you have experienced as the years have gone by, which for some has happened slowly over a number of years and for others seemed to happen over-night. That gradual gain in weight, the change to where you carry it from the hips to around the middle, the constant fatigue, the change to your hair, skin and joints. The muscle pain, the constant lack of energy, loss of libido, hot flushes, loss of concentration, mindfulness and memory, the mood swings and increased anxiety and much more. The list can go on and for some, leads to years of constant despair and a general acceptance of this is how it is going to be now! Read on and you will see that with some specialist assessment and treatment you can change your hormone status.
As a clinical exercise physiologist, I used to think I was exempt these changes. I am sure many healthy eaters, healthy exercisers will have thought the same for years too, then bang. It hits you. Why? I have eaten healthily all my life and exercised as I should. Why have I gained all this weight? Why do I feel exhausted all the time? Etc. For me it has been an interesting personal journey and I know many of you will relate to it.
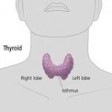 Around the early thirties I was unlucky enough to experience a thyroid condition that meant I had to have a thyroidectomy and the whole of one side of my thyroid and 75% of the other was removed. What I learnt through this period is how many women from mid-thirties may also experience conditions related to the Thyroid and may go through years being undiagnosed. It was only having a specific problem that I discovered mine.
Around the early thirties I was unlucky enough to experience a thyroid condition that meant I had to have a thyroidectomy and the whole of one side of my thyroid and 75% of the other was removed. What I learnt through this period is how many women from mid-thirties may also experience conditions related to the Thyroid and may go through years being undiagnosed. It was only having a specific problem that I discovered mine.
As an exerciser at the time, I felt I didn’t need to take thyroid hormone replacement treatment and managed it for several years by making healthy choices. I even managed to mask the symptoms by living on a stimulant, diet coke. It was a struggle and over the years weight gradually crept on and once I reached early fifties and the menopause hit, the weight increased more.
My thought process was “I know what I am doing though, can I not control this?” “With my level of knowledge surely, I can sort this out. ”As an instructor in our industry this can add to your despair, especially when you read social media comments and posts from fitness professionals who stereotype other professionals who may carry weight as those instructors don’t practice what they preach. You become very self-conscious and believe that this is what everyone thinks. Is that familiar to you or your clients? I find professionally that my thyroid condition is almost the first thing I tell people so that they don’t judge me. It took me a lot of years to understand that there are things you have to accept that you cannot control with food and exercise alone and that you may need more professional help. In fact for me it was coming off diet coke that made my symptoms more evident and forced me to seek professional help. I do wonder how many other women or female clients live with the symptoms and keep themselves functioning by other stimulants as I did.
A low functioning thyroid and the menopause are two of the areas you cannot control and I would recommend you seek specialist help. Whilst being healthy can minimize symptoms and help you cope with symptoms, you cannot exercise or eat the menopause or hypothyroidism away. Why? Well read on.
Let’s try and understand the changes that occur if you experience hypo-thyroidism and or the menopause. Thyroid hormones play an important role in the body. Thyroid hormone deficiencies may be suspected clinically whenever there is a series of symptoms present.
Symptoms
Symptoms may present as severe or mild sub clinical and can often be masked i.e. tiredness can be attributed to other causes. The symptoms can often be missed and can sometimes be attributed to the ageing process or confused with the menopause symptoms by mistake. Symptoms may be mild at first and increase over a number of years also making them easy to miss as you get used to living with them.
| Common Symptoms | Common Symptoms |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Hypothyroidism (under active thyroid) is a consequence of deficient secretion by the thyroid gland of the thyroid hormones T3 (triiodothyronine) and T4 (thyroxine). Hypothyroidism accounts for up to 80% of thyroid disease cases. (Hyper-thyroidism is not the scope of this article)
When working effectively the thyroid hormones travel through the bloodstream and control the rate at which energy in the body is converted (we refer to this as metabolism). The hormones keep the metabolism working at the correct pace. They are also responsible for regulating body temperature and blood calcium levels.
Hypo-thyroidism often presents with non-specific symptoms or symptoms which are masked by other things such as dry skin, tiredness or weight gain. It can be congenital (at birth) or developed in later life. It is classed as primary or secondary. Primary is a dysfunction of the thyroid gland itself and is usually the low-level production of one or more of the hormones or the complete lack of production of one or more of the thyroid hormones. Secondary classifications the pituitary gland (the stimulating gland) or hypothalamic (brain control centre) dysfunction.
Women are much more likely to develop thyroid problems than men. Around 1 in 50 women and 1 in 1000 men develop hypothyroidism at some time in their life. Most commonly it develops as an adult. The most common cause is due to an autoimmune disease called autoimmune thyroiditis. The immune system fails to recognise the gland as being one of your own bodies organs and attacks it with antibodies as if it is a virus. The antibodies then attach themselves to the thyroid and affect its function. It then gradually develops the condition. It can swell and develop into a ‘goiter’. This is then referred to as Hashimoto’s disease.
The condition can also be caused by lack of iodine (not common in a normal UK diet), a side effect of some medications, a pituitary gland problem or a congenital defect (1 in 400 babies are born without a thyroid gland).
Thyroid Physiology
The hypothalamus (brain), pituitary gland and the thyroid gland all play a part in the feedback and regulatory mechanisms involved in the production of thyroxine (T4) and triiodothyronine (T3) from the thyroid gland. It’s a cascade of events leading to full function.
- Thyroid releasing hormone (TRH) is secreted by the hypothalamus (brain) and stimulates the production of the thyroid stimulating hormone (TSH) from the anterior pituitary gland.
- TSH then stimulates the production and release of T4 from the thyroid gland and its conversion hormone T3. T3 is the hormone directly used by the cells
- Once released, T4 and T3 then exert a negative feedback loop mechanism on TSH production. In other words, it signals to the pituitary gland to switch off the production of TSH indicating that everything is functioning normally and effectively
- T4 is the main hormone produced by the thyroid.
- T3 is mainly produced by peripheral conversion of T4.
- T3 and T4 both act to increase cell metabolism. This is the turnover of energy in each cell.
When the thyroid gland doesn’t produce enough thyroxine T4 or conversion to T3 is low, it causes many of the functions of the body to slow down including blood functions.
How is it diagnosed?
Thyroid function testing by blood test is the most common method of diagnosis. This is an endocrine (hormone) function test. Over 10 million tests per year are conducted in the UK at a cost of £30 million. It can be a problematic test and not necessarily diagnose the condition. The mechanism for use of the thyroid hormones is intra-cellular and not utilized by the blood and the test does not test this. There can also be a problem with low blood volume in a hypo-thyroid individual therefore blood panel readings will appear higher.
TSH– The pituitary gland produces the hormone TSH (see above physiology) which is measured in the blood. This hormone stimulates the production of thyroxine (T4). If the levels of TSH are elevated this means the levels of thyroxine are low and the TSH levels are trying to encourage the thyroid to make more.
T4 – if T4 levels are low it is confirmed.
Sometimes you can have normal levels of T4 produced by the thyroid but elevated TSH which means the pituitary is working harder to stimulate the thyroid. This means you may well be what they call sub clinical and develop full hypo-thryoidism in the future.
Getting an accurate test to diagnose hypo-thyroidism can be difficult. After doing tests your doctor may tell you that you are in the “normal range”, even if you still have hypo-thyroid symptoms and know something is very wrong in your body. This could be because you are at the very edge of the range, either at the bottom or at the top, you could be classed as “borderline”. It is difficult to diagnose normal range. Unless you were tested prior to being ill its impossible to know what ‘normal range’ for you would be. One of the questions that baffled me throughout all the years I had tests at the GP was if there is a range and you are at the very bottom of that range how can they class that as normal.
The blood test may not pick up dysfunction at cellular level or be testing level conversion to T3. If you are not converting from T4 to T3 or if your cells are not taking up the T3 normally, your T4 levels and your TSH levels will still show as normal. This is because national health tests do not test for the full range of the hormones as it is very expensive. If you suspect that you may be suffering, then it is better to see a specialist GP.
Thyroid UK believe that you need to know your Free T3 level because this will often show low if you are not converting, and high if you have blocked receptor cells. Even if you are converting, the body needs the extra T3 that a normal thyroid produces.
It is worth asking your doctor to conduct further testing and ensure that they look at the global condition and take your symptoms into consideration.
Treatment
The treatment is to take thyroxine replacement therapy each day to normalize the TSH and obtain a positive thyroid state in the body. To obtain this, FT4 and TT4 have to be maintained at, or just above, the upper reference interval”.This replaces the thyroxine that your thyroid gland is not making. It is also recommended to take Selenium every day and Zinc. Most people feel much better soon after starting treatment however it can take some time to get the dosage correct. The British Thyroid Foundation state that the correct dose is what resumes good health.
Menopause & Hormone
It is a normal process through a stage of life that all women have to look forward to. It is caused by the loss of all the remaining follicles in the ovaries which contain eggs. When the follicles die, the ovaries no longer secrete the hormone oestrogen and progesterone which allow the lining of the womb to build up each month resulting in a monthly period and produces many adverse symptoms discussed below including weight gain. The ovaries become less responsive to two hormones involved in reproduction—Luteinizing Hormone (LH) and Follicle-Stimulating Hormone (FSH). FSH and LH can no longer perform their usual functions to regulate your oestrogen, progesterone and testosterone.
As oestrogen reduces or ceases, the body may seek to convert more calories into fat, in order to increase oestrogen production in the fat cell and it redistributes this from the hips to the abdominal area. This means weight gain.
Low levels of the hormone progesterone may cause water retention or bloating. This can make you feel heavier and makes your clothes fit tighter. Testosterone works to build and maintain muscle mass amongst other things. This helps keep your metabolism high. The reduction of this hormone during menopause causes the loss of muscle mass and hence result in lower metabolism and an increase in weight gain. It all sounds like a downhill slippery slope and an uphill battle.
A few years before the menopause, periods may be haphazard due to perimenopause which can begin as early as five years prior to the full menopause. It usually begins around age 45 to 55. The actual menopause tends to strike at around 50-52 years of age, although the exact timing differs among individuals. You aren’t going to wake up on your 50th birthday with menopause. Some women may experience an early menopause at a young age from a premature ovarian insufficiency or other medical reasons.
- Periods stop
- Hot flushes & night sweats
- Vaginal dryness & loss of muscle tone
- Loss of libido
- Disturbed sleep
- Change in cognitive function (memory)
- Unexplained Weight gain around the midriff
- Irritability and mood swings sometimes leading to depression
- Loss of bone density
Many women may only suffer some of the symptom and others may experience them all, around 80% of women suffer from additional menopausal symptoms as well as the periods stopping. The most common menopausal symptoms are hot flushes and night sweats. These happen most commonly within the first year after the last period, although they can occur earlier. If severe, these can cause weakness and loss of energy, particularly night sweats, which may disturb normal sleeping patterns. Their severity tends to decrease with time.
Decreased production and release of oestrogen can cause vaginal changes such as dryness and loss of muscle tone, which can make sexual intercourse uncomfortable or painful. This, along with sleep or mood changes, can lead to loss of interest in sexual intercourse.
Depression, anxiety, memory issues and panic attacks may also occur. Some women may experience problems with urinary control (incontinence), particularly those who are overweight.
How is it diagnosed?
To diagnose the menopause, a woman should have stopped periods for a minimum of 12 months. Therefore, menopause can only be identified retrospectively. However, there are other symptoms (such as those described above) that can give an indication that a woman is undergoing the menopause, most commonly night flushes in combination with irregular periods. Another method is to measure the levels of hormones such as follicle stimulating hormone in a blood sample. This will be raised just before and after the menopause. This test may not give a decisive result and is not recommended in women who are either over 45 or who are taking the pill but usually indicates the ovaries are no longer secreting oestrogen or progesterone.
Treatment
Menopausal symptoms can be treated with hormone replacement therapy (HRT). For women with a womb (uterus), HRT will contain both oestrogen and progesterone. For women who have undergone a hysterectomy only oestrogen replacement is required. There are many different hormone replacement options such as Bio-Identical HRT which is low dosage HR which replicates your own hormone molecular structure. They can be administered by pills, skin patches, skin gels or implants.
Rather than full HRT I would again recommend seeing a specialist GP who specialises in Bio-Identical HRT, and HRT. High dosage HRT can bring along its own problems and if the dosage is incorrect it can also cause you to gain more weight, tender breasts, water retention, depression and nausea. A specialist GP will be able to take more detailed blood tests and also explore all of the options available.
BHRT requires blood tests to assess your current hormone levels so that personalised, minimal HRT can be prescribed which for you may be a more optimal solution. This may not be an option at your NHS GP as again these tests are more expensive. It is worth the investments. BHRT allows flexibility of prescribing and very closely mimics your natural hormones so that any potential side effects are minimised. They are made from plant sources and are well tested and safe. It gives you a much more tailored solution. When you think how complex our bodies are, I would definitely recommend this more specialist solution.
If you or your clients experience any of the symptoms of either condition or life phase don’t wait, seek that specialist help. Whilst we can help with exercise and good nutrition it won’t necessarily bring you all the relief you will need.
How Can Nutrition Help?
As with all bodily functions (you are what you eat), your diet plays a major role in the health. There are some specific nutrients that your thyroid needs for effective function and it’s important to include them in your diet:
- Selenium: This mineral is an antioxidant mineral and is critical for the proper functioning of all of your body particularly your thyroid gland and is used to produce and regulate the T3 hormone.
Selenium can be found in shrimp, snapper, tuna, cod, halibut, calf’s liver, button and shitake mushrooms and Brazil nuts, sunflower seeds, rice, wheat and oat bran.
- Zinc and Iron: These are needed in tiny amounts for healthy thyroid function, metabolic rate and immune function. Low levels of zinc have been linked to low levels of TSH, whereas iron deficiency has been linked to decreased thyroid efficiency. Zinc can also help with general weight management and help keep weight lower during the menopause.
Foods such as prawns, lamb, grass fed beef, calf’s liver, spinach, mushrooms, sunflower, pumpkin and sesame seeds can help provide these trace metals in your diet.
- Omega-3 Fats: These essential fats (fish oils), play an important role in thyroid function, and any help your cells become sensitive to thyroid hormone.
- A C E Antioxidants and B Vitamins: The antioxidant vitamins A, C and E can help your body combat free radical damage caused by oxidative stress that may damage the thyroid and your general cellular structure. Antioxidants will help keep mitochondrial efficiency higher and help with weight management related to both thyroid and menopause weight gain and muscle mass loss. In addition, B vitamins help to manufacture thyroid hormone and play an important role in healthy thyroid function.
Foods such as fruit and vegetables contain these vitamins
Vitamin Aor retinol is found in liver, animal fats, oils such as olive and soy, cereal grain germs like wheatgerm and egg yolks. Fruit and vegetables contain beta-carotene in their yellow and orange pigments which is converted to vitamin A in your body.
B-complex vitamins. Most of the B-complex vitamins are found in pork, grains, vegetables and milk. Thiamine is found in pork, cheese, dried fruit and peas; riboflavin in small quantities in milk, eggs and mushrooms; and niacin in beef, milk, wheat flour and eggs. Pyridoxine can be found in a wide variety of foods including chicken and turkey, eggs, oatmeal, rice, peanuts and bread. Vitamin B12 is present in most meats, seaweed, salmon, milk, yeast extract and eggs.
Vitamin C or ascorbic acid is found in fresh fruit and vegetables, sweet potatoes and fresh milk. The foods highest in vitamin C are: black currants at 220 mg per 100 g, guavas at 180 mg, bell peppers at 100 mg, cauliflower at 120 mg, cabbage at 120 mg and parsley at 150 mg.
Vitamin E is found in high quantities in nuts, seeds and vegetable oils such as olive and soy.
Menopause
The general advice to eat a healthy, varied diet, based on unrefined foods and plenty vegetables, nuts and grains and low in saturated fat, sugar and salt.
For menopausal and post-menopausal women there are aspects of the diet that are especially important, in order to reduce the risk of developing cardiovascular disease and osteoporosis and to help with day-to-day menopausal symptoms associated with lower levels of oestrogen.
Calcium
Calcium studies have shown that the ability to absorb calcium declines after the menopause. The recommended intake of calcium is 700 mg per day for adults. You should be able to get all the calcium you need from your diet. Important sources of calcium are:
- dairy products, such as milk, yogurt or cheese (go for the lower fat options);
- products fortified with calcium, such as bread (most bread flour is fortified with calcium), breakfast cereals and dairy alternatives (e.g. soya drinks);
- some green leafy vegetables such as watercress and kale (but not spinach);
- sesame seeds;
- dried figs;
- and fish that is eaten with bones (such as sardines).
Vitamin D
Vitamin D declines through the menopause which is linked to the hot flushes due to Vitamin Ds role with the neurotransmitter Serotonin. Oestrogen increases the activity of the enzyme responsible for activating vitamin D and so declining levels during the menopause could lead to symptoms of vitamin D deficiency. Vitamin D can also help improve mood and cognitive function.
Supplements
A number of dietary factors, supplements and herbal remedies have been suggested to be of benefit in relieving symptoms of the menopause. In particular there has been a lot of interest in the role of phytoestrogens (the two main types are isoflavones and lignans) as they are similiar in structure to oestrogen and therefore may help to alleviate some of the symptoms of low oestrogen levels associated with the menopause. These substances are found in plants.
- Dietary sources of isoflavones include soyabeans, legumes, lentils and chickpeas and foods made from these such as texturised vegetable protein, tofu and soya drinks.
- Dietary sources of lignans include cereals, linseeds and fruit and vegetables.
There is some evidence that consuming isoflavones in foods or as supplements can help to reduce the menopausal symptoms of hot flushes and vaginal dryness. However, more studies are needed to confirm whether isoflavone supplements are safe and effective in reducing menopause symptoms.
There are a range of herbal remedies on the market claiming to combat menopausal symptoms but currently there is a lack of scientific studies on their safety and effectiveness. Speak with your GP before taking any of these as they may have side effects or interact with other medications.
(reference The British Nutrition Foundation)
Following a healthy eating plan for hormonal balance is the key to health and especially during and post menopause and if you are suffering from any Thyroid related conditions. This includes unrefined food, oily fish, lean meats, lots of vegetables particularly root vegetables, seeds and nuts. For further information or an eating plan to follow contact www.drummondclinic.co.uk
How can exercise help?
Regular exercise is important to maintain good health. It is especially important in the treatment of hypothyroidism and menopause to maintain a healthy weight. Exercises increases tissue sensitivity to the thyroid hormone, stimulates normal hormone secretion and improves respiratory function. Exercise will also help retain muscle mass during menopause, reduce bone mineral density loss and increase metabolic output and increase cardio respiratory fitness and help prevent heart disease. Exercise can also help control stress which can help normalise all hormone control. Exercise will help combat the symptoms of fatigue and improve the metabolism and overall feeling of well being.
An exercise regime of between 15-20 minutes per day initially will be beneficial increasing as you progress to 40 minutes per day. This exercise should include cardiovascular training and muscle conditioning.
Cardio-vascular
Exercising at low intensity can increase blood levels of T3, T4 and TSH. This can include interval training, aerobics, dance, walking, swimming and cycling. Low to moderate intensity CV will help maintain heart health during and post menopause and help with oxygen carrying capacity and bone health.
Muscle Conditioning
Improving muscle tone particularly in the slow twitch muscle fibres (type 1) which are the aerobic fibres and the fast twitch type A which are also aerobic will help increase metabolism. Low to moderate resistance training working compound functional movement patterns is the most effective form of training. Moderate strength training will help maintain muscle mass and keep metabolism high.
If you train female clients who are coming up to the age of menopause or have been experiencing any of the symptoms described above. Share this article with them and discuss the challenges they may face and help them understand what is happening and what they can do about it.
If you would like to learn more about nutrition and receive a free registration to the Carbohydrate Pyramid healthy eating plan then book your nutrition course place today.

